Man Survives 48 Hours Without Lungs in a Medical First
An artificial lung system sustained a patient for 48 hours without lungs, enabling a life-saving double transplant and highlighting the need for earlier intervention in severe ARDS.
People cannot survive without lungs. Yet one of Ankit Bharat’s patients did so for two full days.
In a study published in the Cell Press journal Med, surgeons detailed how they extracted a patient’s severely infected lungs and relied on a custom-built “artificial lungs” setup to sustain him until donor organs became available. The team describes the strategy as a potential bridge to transplantation for patients who would otherwise die waiting.
“He was critically ill. His heart stopped as soon as he arrived. We had to perform CPR,” recalls Bharat, the lead author and a thoracic surgeon at Northwestern University. “When the infection is so severe that the lungs are melting, they’re irrecoverably damaged. That’s when patients die.”
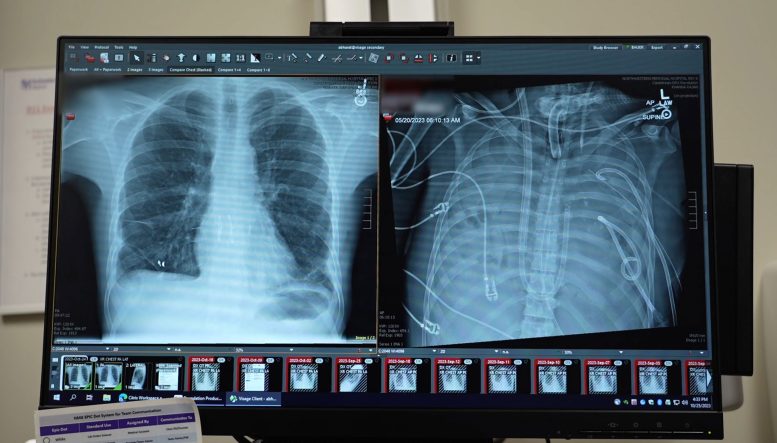
Severe ARDS and Multi-Organ Failure
The patient was a 33-year-old man diagnosed with acute respiratory distress syndrome (ARDS), a dangerous condition in which intense inflammation and infection flood the lungs. His illness began with the flu and rapidly worsened, compounded by bacterial pneumonia. As his lungs failed, his heart and kidneys also began to shut down. Doctors determined that a double lung transplant was his only realistic chance to survive.
His lungs were beyond saving and were continuing to drive infection throughout his body. At the same time, he was too unstable to immediately undergo transplantation. His body needed time to recover before it could handle new organs.
“The heart and lungs are intrinsically connected,” says Bharat. “When there are no lungs, how do you keep the patient alive?”
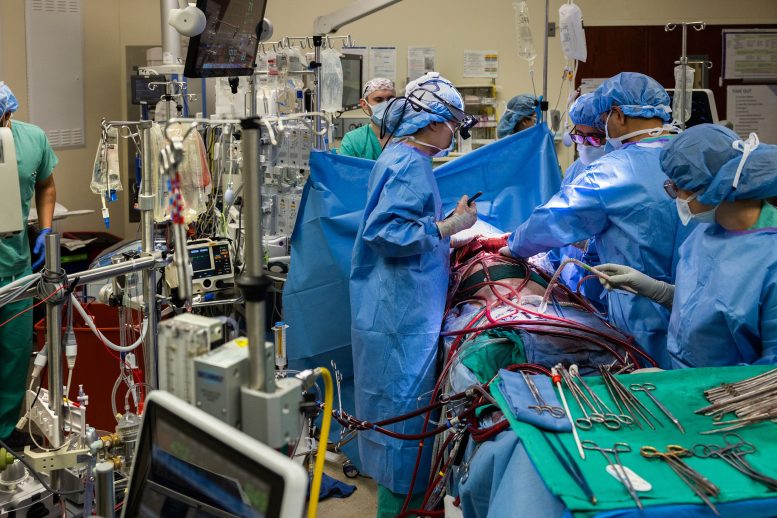
Engineering an Artificial Lung Bridge
To buy that time, Bharat and his colleagues created a system that could temporarily perform the essential tasks of the lungs. The device added oxygen to the blood, cleared out carbon dioxide, and supported circulation so the heart could keep pumping effectively, even in the complete absence of lungs.
After surgeons removed the infected organs, the patient’s health began to rebound. His blood pressure steadied, his other organs started functioning again, and the infection came under control. Two days later, compatible donor lungs were found, and the team carried out a double lung transplant. More than two years after the operation, he is back to his normal routine with strong lung function.
“Conventionally, lung transplant is reserved for patients who have chronic conditions like interstitial lung disease or cystic fibrosis,” says Bharat. “Currently, people think if you get severe ARDS, you keep supporting them, and ultimately the lungs will get better.”
Molecular Evidence for Early Transplant Decisions
However, examination of the removed lungs suggested that recovery would never have happened. Detailed molecular testing revealed extensive scarring and significant immune-related injury. These findings indicated that the damage had progressed too far for the tissue to heal.
“For the first time, biologically, we are giving molecular proof that some patients will need a double lung transplant; otherwise, they will not survive,” says Bharat.

At present, only a few highly specialized hospitals have the skill and resources to perform this type of procedure. Bharat hopes that in the future, more standardized devices will be developed to help sustain patients with catastrophic lung failure while they wait for donor organs.
“In my practice, young patients die almost every week because no one realized that transplantation was an option,” Bharat says. “For severe lung damage caused by respiratory viruses or infections, even in acute settings, a lung transplant can be lifesaving.”
Reference: “Bridge to transplant using a flow-adaptive extracorporeal total artificial lung system following bilateral pneumonectomy” by Yuanqing Yan, Anitha Chandrasekhar, Hee Chul Yang, Teja Devarakonda, Aaron Reynolds, Anjana V. Yeldandi, Ambalavanan Arunachalam, Chitaru Kurihara, G.R. Scott Budinger and Ankit Bharat, 30 January 2026, Med.
DOI: 10.1016/j.medj.2025.100985
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
link



