A chronic multidimensional measure of energy poverty and its impacts on physical and mental health
Baseline results
We adopt the regression model used in most of the literature to test the impact of chronic multidimensional energy poverty on health with the following model specification:
$$Healt{h}_{i}={\beta }_{0}+{\beta }_{1}CME{P}_{i}+{\beta }_{2}{X}_{i}+{\beta }_{3}{F}_{i}+{\beta }_{4}Pr{o}_{i}+\varepsilon$$
(6)
where Healthi denotes the health status of individual i (including both physical and mental health) and CMEPi denotes the chronic multidimensional energy poverty index. Xi is a vector of individual characteristics, Fi is a vector of household characteristics, Proi is a provincial fixed effect, and ε is a randomly distributed error term. The coefficient β1 is the central concern of this study. When the dependent variable is Physical, the coefficient β1 is significantly negative, which implies that chronic multidimensional energy poverty has a significantly negative effect on an individual’s physical health. When the dependent variable is Mental, the coefficient β1 is significantly negative, which implies that chronic multidimensional energy poverty has a significantly negative effect on the individual’s mental health.
Table 6 presents the regression results. Columns (1) and (2) use physical health as the dependent variable, with the former controlling for individual characteristics only and the latter adding family characteristics. In both models, the coefficients on CMEP are negative and significant at the 1% level, indicating that chronic multidimensional energy poverty significantly harms physical health, with higher levels associated with poorer self-reported health. Columns (3) and (4) use mental health as the dependent variable under the same control settings. The coefficients on CMEP are positive and significant at the 1% level, suggesting that chronic multidimensional energy poverty also deteriorates mental health. Specifically, higher levels of deprivation are associated with increased Ces-d-8 depressive symptoms, reflecting greater psychological harm.
Consistent with previous studies (e.g., Zhang et al. 2019; Kose 2019), Table 5 shows that age, gender, and employment status are related to health. Family size and number of children have a significantly positive effect on both physical and mental health, aligning with Kendall and Anglewicz (2018) and studies linking family size to lower depressive symptoms (Nie et al. 2021). Other controls show that education, marital status, and urban–rural residence are not significantly related to physical health but do affect mental health. Education enhances cognitive abilities and social status, reducing depression (Lee 2011). Marriage may improve psychological health through companionship and support. Urban residents benefit from better infrastructure, services, and higher income, which can reduce depression (Huang et al. 2017). Poverty alleviation policies and improved rural medical insurance have narrowed urban–rural differences in physical health (Fang et al. 2019), explaining the lack of a significant relationship between residence and physical health in this study.
Endogeneity
While the baseline regression establishes a significant relationship between CMEP and residents’ physical and mental health, concerns regarding endogeneity remain. These concerns primarily stem from two sources: reverse causality and omitted variable bias. Poorer health conditions may reduce income-earning capacity, limiting access to modern energy sources. Omitted variable bias occurs when unobserved factors, such as regional development disparities or household preferences, simultaneously affect both CMEP and health outcomes, leading to biased estimates.
To address these endogeneity concerns, we employ the instrumental variable (IV) approach following Lewbel (2012), combined with a two-stage least squares (2SLS) regression. This method allows for the generation of internal instruments based on heteroscedasticity, providing a viable solution when traditional IVs are unavailable. Additionally, we incorporate external instruments derived from exogenous policy shocks—specifically, the Carbon Emission Trading Policy (CETP) and the New Energy Demonstration Policy (NEDP). CETP, introduced in 2013 across pilot regions such as Beijing and Tianjin, aims to enhance energy efficiency and reduce carbon emissions. NEDP promotes the adoption of renewable energy technologies. The validity of these policies as instruments lies in the fact that, while they do not directly affect individual health, they influence household energy choices and affordability, thereby impacting CMEP.
Our empirical strategy follows a stepwise approach. First, we implement the Lewbel internal IV method and, subsequently, extend the analysis by incorporating external IVs based on CETP and NEDP. A key requirement for the validity of the Lewbel IV approach is the presence of heteroscedasticity, which we confirm through the Pagan–Hall and Breusch–Pagan tests. Table 7 reports the results of these endogeneity tests, showing strong statistical evidence of heteroscedasticity, thereby justifying the use of this method. Additionally, the first-stage F-statistics consistently exceed 10 across all specifications, indicating the absence of weak instrument bias.
The IV regression results are presented in Table 7. Columns (1) and (2) report the estimates using the Lewbel internal IV, confirming that CMEP continues to exert a significant negative impact on both physical and mental health. Columns (3) through (6) present the results incorporating external IVs, separately examining CETP and NEDP. The findings remain robust across all specifications, reinforcing the conclusion that the adverse health effects of CMEP persist even after addressing potential endogeneity concerns.
Robustness checks
Replace the dependent variable
To address potential bias from measurement errors in health indicators, we perform robustness checks using physical health from medical examinations and life satisfaction as complementary measures for physical and mental health. In the CFPS dataset, physical health is assessed on a seven-point scale based on self-reported evaluations after a medical examination, providing a more structured measure than subjective health assessments. Life satisfaction, measured on a five-point scale, serves as a proxy for mental health, consistent with prior studies linking it to psychological well-being (Nie et al. 2022). Table 8 presents the results. Column (1) shows that chronic multidimensional energy poverty significantly worsens physical health, with a positive coefficient significant at 1%. Column (2) indicates a negative coefficient significant at 10% for life satisfaction, suggesting that higher energy poverty reduces mental well-being.
In the baseline regression, we used 2018 physical health attitudes and Ces-d-8 depressive scores as proxies for physical and mental health, implicitly assuming continuous incremental effects. To address potential measurement errors, we instead use the mean values of these indicators across four observation periods in columns (3) and (4). Both coefficients on CMEP remain significant at 1%, confirming that individuals in severe long-term energy poverty exhibit poorer physical and mental health. The smaller magnitude compared to the baseline reflects the smoothing effect of averaging over multiple periods, as expected.
Adding control variables
Omitted variable bias arises when relevant factors are excluded from the model, potentially distorting the relationship between independent and dependent variables. In our study, economic factors such as household income and consumption expenditure may influence both CMEP and individuals’ physical and mental health, potentially confounding the results. By including household income and consumption expenditure as controls, we account for the broader economic context shaping health outcomes. These variables reflect a household’s resources, which affect access to healthcare, nutrition, and other services critical to health (Tang et al. 2024; Shen et al. 2025). Controlling for them ensures that the estimated effect of CMEP is not conflated with underlying economic poverty.
The results, shown in columns (5) and (6) of Table 8, indicate that even after controlling for these economic factors, the coefficient of CMEP remains significant at the 1% level. This finding provides strong evidence that the relationship between CMEP and health outcomes is robust and not simply driven by underlying economic factors such as income or consumption expenditures. In other words, even after accounting for the potential confounding effects of economic poverty, CMEP continues to exert a significant impact on both physical and mental health, further reinforcing the validity of our conclusions.
Change the estimation method
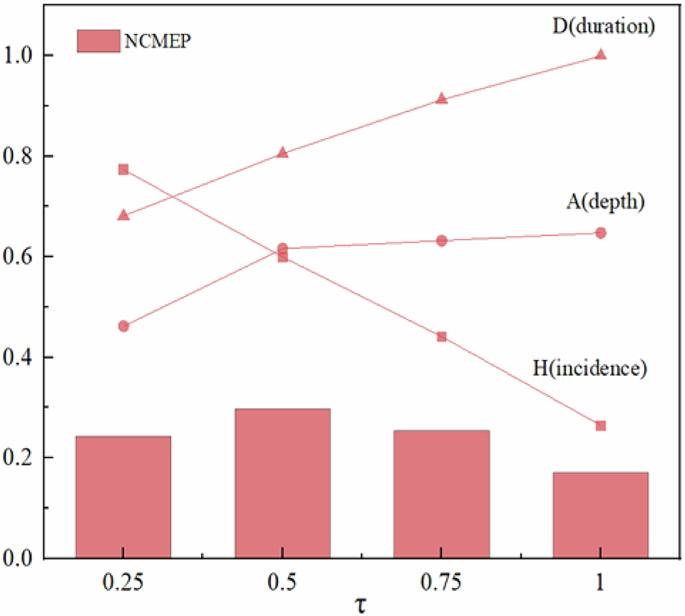
We change the estimation method to propensity score matching (PSM), which has the advantage of including fewer model constraints and mitigating sample self-selection bias on observable variables (Wang et al. 2025). Using the PSM method first requires the discretization of the chronic multidimensional energy poverty index. We select the time threshold \(\tau\) for chronically multidimensionally energy-poor households as the classification criterion. To ensure robustness, we apply four matching methods—nearest neighbor, radius, kernel, and local linear regression—using the same control variables as in the baseline regression.
Table 9 reports the PSM results. We focus on the average treatment effect on the treated (ATT). For physical health, ATT is negative, indicating lower health attitude scores among chronically multidimensionally energy-poor households compared to non-poor households. For mental health, ATT is positive, indicating higher depression scores among the chronically energy-poor. Across all matching methods and poverty criteria, the core ATT remains significant at the 1% level, confirming that chronic multidimensional energy poverty substantially impairs both physical and mental health.
Adjusting measurement weights
Since the baseline model uses equal weighting for the dimensions of long-term multidimensional energy poverty, it is crucial to assess whether different weightings for these dimensions could lead to significant variations in the results. The concern arises from the possibility that certain dimensions of energy poverty, such as energy accessibility or affordability, may have stronger effects on residents’ physical and mental health than others, thus altering the overall impact when given different weights.
To address this issue, we re-estimate the CMEP index by adjusting the weights assigned to each dimension, thereby shifting from an equal-weighted structure to schemes that emphasize one dimension over the other. We then rerun the regression analysis using the modified CMEP indices to assess whether the results remain robust. Table 10 reports the outcomes of this sensitivity analysis. The results indicate that, under all alternative weighting schemes, the estimated effects of chronic multidimensional energy poverty on both physical and mental health remain statistically significant. This consistency across specifications reinforces the reliability of the findings and suggests that the negative association between long-term multidimensional energy poverty and health outcomes is robust to variations in the relative importance assigned to its constituent dimensions.
Mechanism analysis
This study’s mechanism analysis examines how long-term multidimensional energy poverty affects individual health through food expenditure and perceived environmental pollution, highlighting the indirect and interconnected pathways linking energy poverty to physical and mental well-being. Food expenditure is a key mechanism. Existing research consistently shows that energy-poor households face constrained budgets, forcing them to make trade-offs between essential expenses such as energy, food, and healthcare (Fry et al. 2023). In these households, energy costs are often prioritized, resulting in reduced food budgets. This effect becomes more pronounced under long-term energy poverty, where sustained financial pressure limits resources over extended periods (Nie et al. 2021). Consequently, households may opt for cheaper, less nutritious food alternatives instead of higher-quality options, leading to adverse health effects due to inadequate nutrition (Sambodo and Novandra 2019).
Perceived environmental pollution is another critical mechanism. Households lacking access to clean energy sources frequently rely on solid fuels like coal, wood, or biomass for cooking and heating. These fuels release indoor air pollutants, such as carbon monoxide and particulate matter, which are linked to respiratory and cardiovascular conditions, including asthma and chronic obstructive pulmonary disease. Beyond indoor effects, the use of such fuels contributes to outdoor air pollution, further degrading environmental quality. This persistent exposure to polluted conditions not only impairs physical health but also affects mental well-being, as poor air quality is associated with increased stress and anxiety, particularly among those with limited means to mitigate their circumstances (Liddell and Guiney, 2015).
To empirically examine these mechanisms, this study uses household food expenditure and environmental pollution as mediators in a mediation analysis, with results presented in Table 11. The findings show that food expenditure significantly mediates the relationship between energy poverty and health: long-term multidimensional energy poverty reduces food expenditure, while higher food expenditure is associated with better health outcomes, reflecting households’ ability to afford more nutritious food when resources allow. Similarly, the analysis confirms that prolonged energy poverty intensifies environmental pollution, further contributing to health deterioration. In summary, food expenditure and perceived environmental pollution are key mechanisms linking long-term multidimensional energy poverty to individual health.
Heterogeneity analysis
Heterogeneity of the individual characteristics
Much of the literature has found that personal characteristics have a significant impact on health (e.g., Hu et al. 2016; Black et al. 2017), and to explore the impact these characteristics have on our results, we conducted a further heterogeneity analysis. Black et al. (2017) examined the importance of age, cognitive ability, and socioeconomic status on health disparities using data from the Australian Household Longitudinal Survey and found significant differences in self-reported health across individuals of different ages and education levels. On this basis, we conjecture that the effect of chronic multidimensional energy poverty on health will show different variability according to respondents’ age and income. To check this conjecture, we conducted the following heterogeneity analysis.
(1) Age. Columns (1) and (2) of Table 12 report the results of the interaction term based on age. The coefficients on the interaction terms for respondents aged up to 50 years pass the 1% significance level test, thus indicating that increasing age strengthens the negative impact of chronic multidimensional energy poverty on health—that is, that respondents aged up to 50 years are more vulnerable to the effects of chronic multidimensional energy poverty on health. This result is consistent with our perception that older people have unique physical and psychological vulnerabilities due to aging and their social circumstances. When living in energy poverty for long periods of time, deterioration in the living environment may further induce illness, and extreme heat or cold temperatures may even increase isolation, anxiety, and fear.
(2) Income. Columns (3) and (4) of Table 12 report the results of the interaction term based on income classification. In the data processing, we define income below the mean as lower income and above the mean as higher income. The results show that the interaction term coefficients for the lower-income group pass the significance test at the 1% level. Low-income respondents are more likely to be negatively affected when their health status is exposed to chronic multidimensional energy poverty, which aligns with previous research (Churchill and Smyth 2021) that shows that lower-income groups are less able to cope with adverse living conditions than higher-income groups.
Regional heterogeneity
China’s vast geographical expanse, shaped by diverse topography, climate, and economic conditions, leads to notable regional variations in the dynamic characteristics of multidimensional energy poverty (see Fig. 3). Given the disparities in economic development levels between China’s eastern, central, and western regions, the spatial and temporal distribution of multidimensional energy poverty is likely uneven. To explore these variations, this study divides the sample into eastern, central, and western regions and examines the heterogeneous effects on the physical and mental health of residents in these areas.
The regression results in columns (6) and (7) of Table 12 reveal distinct patterns. Long-term multidimensional energy poverty significantly reduces physical health in eastern and central provinces, whereas its effect in western provinces is statistically insignificant. Regarding mental health, energy poverty increases depression levels across all regions, with the western provinces showing a statistically significant difference compared to the central region. These results indicate that the health consequences of energy poverty vary by region.
Regional differences in adaptability to air pollution, influenced by geographic and socioeconomic conditions, help explain these effects (Ji et al. 2022). In the more developed eastern and central provinces, households lacking access to modern energy often rely on coal and similar fuels, producing indoor air pollution that harms physical health and may worsen mental health over time. In contrast, residents in the western region, dominated by heavy industry, appear less sensitive to energy-related pollution in terms of physical health—likely due to adaptation to chronically high pollution—but this adaptation does not mitigate the mental health impact, as depression levels remain elevated.
link